The skin is the body’s first line of defence against infection. Multiple layers of the skin like the epidermis, dermis and subcutaneous layer provide various types of protection. All the skin layers work together to prevent skin infections.
A small cut is enough to allow an invading microorganism to enter the skin. This is how a skin infection frequently begins.
Sometimes the cut is not so small, such as after surgery. When the skin is injured somehow, it is more vulnerable to infections.
What is a skin infection?
Infections are typically caused by one of the three organisms, namely, bacteria, virus or fungi. Yeasts and parasites are also known to cause infections.
Most organisms are harmless on the skin’s surface. Bacteria are usually abundant on all human skin. However, trouble can ensue when they enter the skin through a cut.
Skin infections can sometimes occur when the microorganisms infect the deep tissues beneath the skin.
Cellulitis is a skin infection that causes redness, swelling and pain in the infected area. Skin abscess or boil is the collection of pus under the skin and is another type of skin infection.
Causes and types of skin infection
The types of skin infections are categorised based on the organism causing the infection.
Bacterial skin infections
Bacterial skin infection occurs when bacteria enter the skin through hair follicles or tiny skin breaks. This can be caused by wounds, scrapes, cuts, surgery, sunburn, burns, animal or insect bites and preexisting skin disorders.
Bacterial skin infection can range in size from a small spot to the entire body surface. They can also range in severity, from harmless to life-threatening. Common bacterial skin infections are
- Staphylococcal infections
- Cellulitis
- Impetigo
Viral skin infections
Viral skin infections encompass a wide range of conditions. They can be a reaction to a virus within the body or a skin infection.
They range from completely harmless to quite severe (but not usually life-threatening). Some are contagious, while others are not dangerous even when touched.
Viral skin infections include,
- Shingles
- Warts
- Herpes simplex
Fungal skin infections
Fungal skin infections can cause skin rashes. They usually manifest as itchy, red, circular rashes and thick, discoloured, flaky nails.
Some fungal skin infections are
Parasitic skin infection
Epidermal Parasitic Skin Diseases (EPSDs) are a diverse group of infectious diseases caused by parasites in the upper layer of the skin. The infection manifests on the skin as a red, bumpy and itchy rash.
Infections caused by parasites include
- Body lice
- Head lice
- Scabies
Skin infections
Skin infections occur when viruses, fungi, parasites or bacteria penetrate and spread through the skin.
Boils
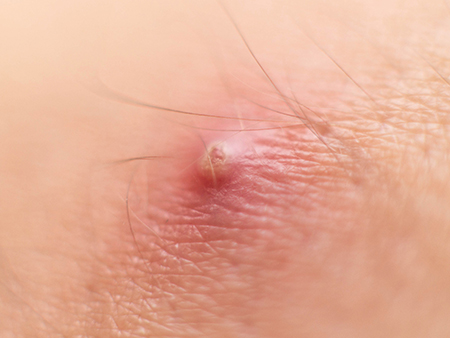
Boils, also known as skin abscesses, are deep and localised bacterial skin infections caused by Staphylococcus aureus. It starts as red, sore spots and develops into bumps with pus. Boils are not contagious in and of themselves, but the pus and liquid inside the boil containing the bacteria can infect the person affected and those in contact.
Impetigo
Impetigo is also a bacterial skin infection that causes blisters or sores on the face, neck and hands. It also affects the diaper area in kids.
Cellulitis
Cellulitis is a deep skin bacterial infection. The hands and legs are the most commonly infected region. It can also appear on the belly and around the eyes, mouth and anus.
Cellulitis can affect normal skin, but it usually occurs when an injury causes a skin break, such as an accident or surgery. Bacteria can go into the skin through cuts and cause infection.
Ringworm
Ringworm is a fungal skin infection. The fungi can cause mild yet bothersome rashes. Fungal skin infections are also referred to as tinea infections.
Ringworm occurs when fungus grows anywhere on the body. It begins as a red, scaly patch or bump on the skin.
Ringworm on the scalp may begin as a small pimple-like sore before becoming patchy, flaky or scaly. Those on the nails can affect one or more fingers or toes.
Jock itch is a form of ringworm that occurs when fungus grows in the groin, upper thighs and buttocks. The athlete’s foot is when the fungus grows on the feet.
MRSA
Methicillin-resistant Staphylococcus aureus is abbreviated as MRSA. MRSA infections begin as small red bumps that quickly develop into deep, painful abscesses.
MRSA is a Staph skin infection that commences as swollen, painful bumps resembling pimples that are warm when touched.
Eczema
Eczema is an inflammatory skin condition that is not contagious. It is a chronic disease that causes dry, itchy skin that can ooze clear fluid when scratched.
Eczema is typically characterised by itching, redness and scaliness.
Symptoms of skin infection
Symptoms depend on the cause of the skin infection.
Pus
Boils are usually a pocket of pus. They typically resemble a pimple but are much larger and go deeper into the skin.
Pus is formed as a result of the body’s immune response to an infection by producing a barrier around it. White blood cells, bacteria and dead cells make up the pus.
Red skin around the injury
Red skin surrounding a wound is due to the natural inflammatory process to heal the injury.
Initially, it is slightly red, and the redness gradually disappears in about a week. Expanding wound and a deep redness imply skin infection.
A red streak
Infection in the skin or subcutaneous tissue is indicated by redness on the skin. This is also a sign that the infection is spreading. Red skin is accompanied by pain, swelling and tenderness.
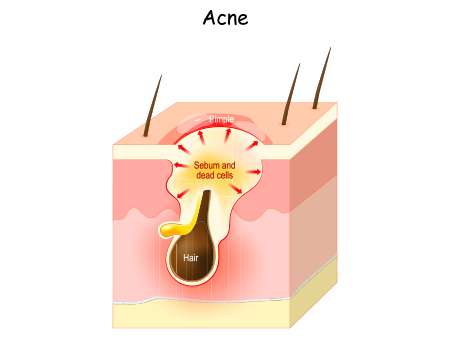
A pimple or yellowish crust on top
When pus builds up in a scab, yellow crusting is formed. Bacterial infections like impetigo or viral infections like herpes are manifested by the pus.
The scab can break in some cases, and yellow fluid oozes out. The yellow liquid is usually serum. Pimples develop on the wound.
Infection is indicated when the yellow scab is swollen or inflamed.
Sores that look like blisters
Bacterial infections like impetigo manifest in the form of blisters. Cold sores can be due to the herpes simplex virus and are accompanied by pain. They tend to break and ooze in a day or two. The blister spots also heal within a couple of weeks without scarring.
Pain
Pain occurs in the infected area in the bacterial skin infection called cellulitis. This is because the infection spreads into deeper layers of the skin. The pain worsens as the days pass.
Swelling
Fluid buildup or inflammation causes swelling. Though swelling happens internally, it affects the outer skin.
The body’s immune system stimulates an inflammatory response to an infection which is noticeable in the form of swelling in the area of infection. This is also common in cellulitis.
Fever
A fever indicates the immune system response where the body tries to fight off the microorganism causing it. It is tough for bacteria or viruses to survive during fever due to high temperatures. However, a very high fever should be taken care of.
The wound hasn’t healed after ten days
A chronic wound may be swelled and change in colour, which produces a foul smell and numbness. Consulting a doctor or dermatologist is the only way to treat a prolonged injury. A wound that wouldn’t heal for four weeks or above needs special attention.
Treatments for skin infection
The treatment is according to the type of infection and its severity. Few infections resolve on their own.
Treatment may include the application of a cream or lotion to the skin. Other treatment options include medications and a procedure to drain pus.
Antibiotics
Antibiotics are only required if the following skin infection symptoms are present.
- Pus-filled bumps
- Pus-oozing cracks, sores or wounds
- Feeling extremely hot or cold
- Fever
- Increased white blood cell count
- Red, warm, painful or swollen wound.
Cellulitis mostly requires antibiotic treatment. A few other skin conditions are also treated with oral antibiotics.
Common oral antibiotics are
- Dicloxacillin
- Tetracycline
- Erythromycin
Cellulitis is best treated with beta-lactam antibiotics, which include penicillin or cephalosporin. For widespread use, beta-lactam drugs are safer than clindamycin.
Clindamycin and TMP-SMX medications are primarily used for boils or draining wounds with a high likelihood of MRSA rather than being used for every uncomplicated skin infection.
Antivirals
Topical antivirals are used to treat the following condition:
- Cold sores or blisters on the lips or face (herpes)
- Infection with the herpes simplex virus of the skin, mucous membrane and genitals.
- Shingles
Antivirals work by preventing infection or limiting the spread of infection.
They cannot cure the viral infection as they are unable to kill the virus, but they may help reduce the pain caused by the sores, hasten the healing process and reduce the healing time.
Commonly used antiviral drugs are
- Aciclovir
- Valaciclovir
These medications can be administered orally, intravenously or topically. Furthermore, they cannot stop the virus from spreading to others.
Topical antivirals should be applied several times a day. Five to six times a day and every three to four hours are usually preferable.
Antifungal creams, ointments, powders
Antifungal medications work by either destroying or inhibiting the growth and multiplication of fungal cells.
These are prescribed to treat fungal skin, scalp and nail infections.
Antifungal medications to treat skin infections include
- Econazole (cream)
- Miconazole (cream, spray powder, powder)
- Griseofulvin (spray)
- Ketoconazole (cream)
- Terbinafine (cream, gel, spray, solution)
Risk factors for skin infection
Injury to the skin
Skin infections are frequently caused or exacerbated by a break in the skin, particularly those that lead pathogens into the dermis. Cuts and other skin breaks can become infected when bacteria enter and multiply in the wound.
Skin conditions, such as athlete’s foot or eczema
Since atopic eczema can cause the skin to become cracked and broken, there exists a risk of bacterial infection. If eczema is scratched or treatment is not correct the risk increases.
Chronic swelling of the legs or arms
Swollen arms or legs are usually noticed in patients with cellulitis. An infection can occur when there is a cut on the swollen skin.
Obesity
Retained moisture in body folds promotes the growth of bacteria and fungi, resulting in skin rashes and infections.
Obese patients are more likely to develop skin infections such as candidiasis, folliculitis, erythrasma, furunculosis and tinea cruris.
According to an article titled ‘Skin changes in the obese patient’, obesity has been linked to an increase in bacterial and candida skin infections. It also states that there is a high incidence of onychomycosis, inflammatory skin diseases and chronic dermatoses such as hidradenitis suppurativa, psoriasis and rosacea.
Diabetes
High blood sugar levels can cause dry skin and weaken the immune system.
Candida albicans are frequently the cause of fungal infections in people with Diabetes. Skin infections caused by the bacteria Staphylococcus aureus are more common and severe in people with uncontrolled Diabetes.
Prevention of skin infection
Skin infection can be prevented by practising the following steps.
Wash your hands often and properly
Washing hands prevents germs from hands that touch other areas, thereby hindering the transmission of microorganisms that cause infection.
Wash scrapes, cuts and wounds
The risk of skin infections is reduced, and the healing process is enhanced when the wounds, cuts and scrapes are adequately washed.
Do not share items
Refrain from sharing items like towels, toys, soaps, razors, toothbrushes and washcloths as the chance of transmitting infection-causing pathogens or existing infection to another person is high.
Avoid skin-to-skin contact with anyone who has a skin infection
Infections spread through contact with infected skin or exposure to infected fluids. To prevent infection, prolonged skin-to-skin contact with infected patients must be avoided.
When to see a doctor?
Consulting a doctor or dermatologist becomes necessary when noticeable changes occur in the skin, particularly if they are blistered, itchy or painful.
The following people are more prone to skin infections.
- Diabetics
- Elderly
- People with poor circulation
- Patients with immune disorders
- Obese people and
- Paralysed individuals.
People falling under these categories must check their bodies on a daily basis and consult a dermatologist if any skin problems or concerns are visible.
Conclusion
Skin infection occurs when microorganisms such as viruses, fungi, bacteria or parasites penetrate the skin and spread.
Some common skin infections are cellulitis, boils, impetigo, folliculitis, MRSA and herpes. Usual symptoms include pus formation, redness, swelling, pain and fever.
Treatment is determined by the type of infection and its severity. Antibiotics, antifungal medications and antivirals are prescribed to treat skin infections.
Doctor consultation is necessary when sudden changes in the skin occur or when the existing infection becomes severe.
FAQs
How can we prevent common skin problems?
Skin problems are prevented by being hygienic. It includes washing hands, maintaining social distance from people having an infection and not sharing personal items.
How do doctors treat skin infections?
Doctors treat skin infections by prescribing antibiotics, antifungal and antiviral medications. These can be oral or topical drugs.
Why do I keep getting skin infections?
Recurrent skin infections may indicate a poor immune system of a person. It may also be due to frequent exposure to microorganisms and unhygienic practices. Cuts in the skin or preexisting infections make a person prone to skin infections.
What is the most common bacterial infection of the skin?
The most common cause of skin infection is Staph bacteria which causes boils. According to a book published in NCBI, cellulitis is a common bacterial skin infection.
Boils and cellulitis are common bacterial infections.
DISCLAIMER: THIS BLOG/WEBSITE DOES NOT PROVIDE MEDICAL ADVICE
The Information including but not limited to text, graphics, images and other material contained on this blog are intended for education and awareness only. No material on this blog is intended to be a substitute for professional medical help including diagnosis or treatment. It is always advisable to consult medical professional before relying on the content. Neither the Author nor Star Health and Allied Insurance Co. Ltd accepts any responsibility for any potential risk to any visitor/reader.





